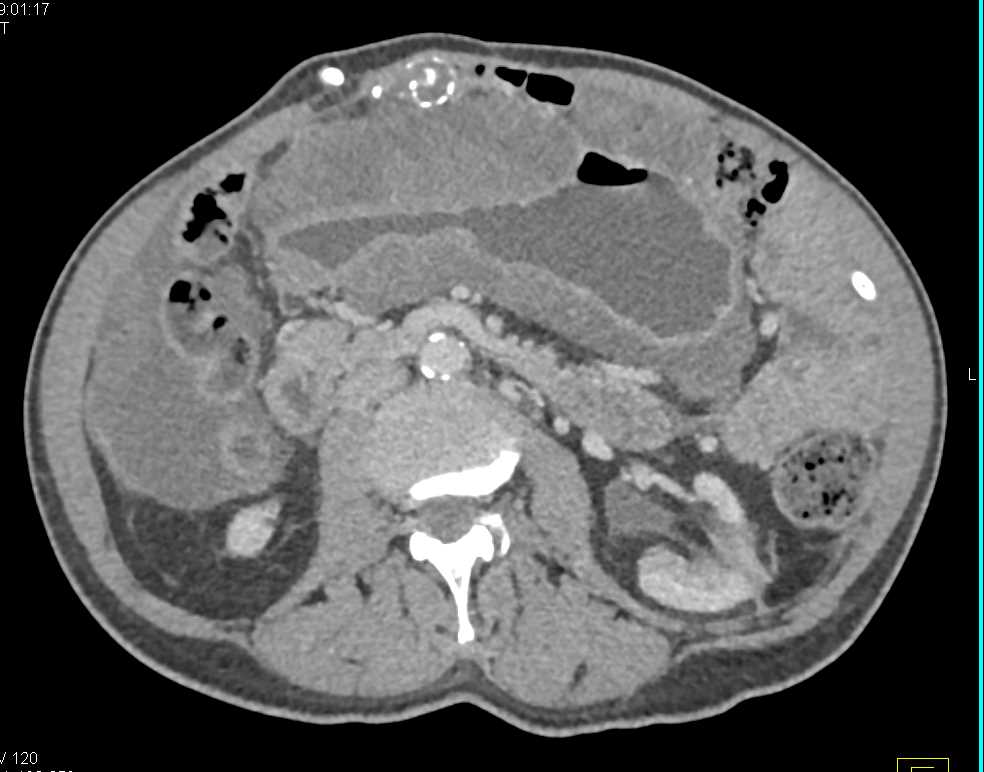
Patients were evaluated regarding age, sex, symptom duration, major complaint, surgical procedure performed, pathologic diagnosis, and their follow-up outcomes. At the second step, we separated these patients as malignant and benign neoplasms of the appendix by using ICD-10 codes C18.1 and D12.1 from the hospital electronic database system.
Pmp cancer code#
At the first step, we searched the patient list for ICD-10 code K35. Patients and Methodsĭuring the study period from January 2003 to August 2013, patients with the diagnosis of AMT were identified from the Vilnius University Hospital Santaros Clinics electronic database using International Classification of Disease 10th revision (ICD-10) codes. The purpose of this study was to evaluate preoperative and postoperative characteristics as well as long-term outcomes of patients with appendiceal mucinous adenomas and PMP. Several investigators have proposed different classifications with similar terminology to describe lesions of variable biologic potential. PMP is the worst complication of AMT, caused by spontaneous or iatrogenic perforation of the appendix, which comes along with a high rate of morbidity and mortality.
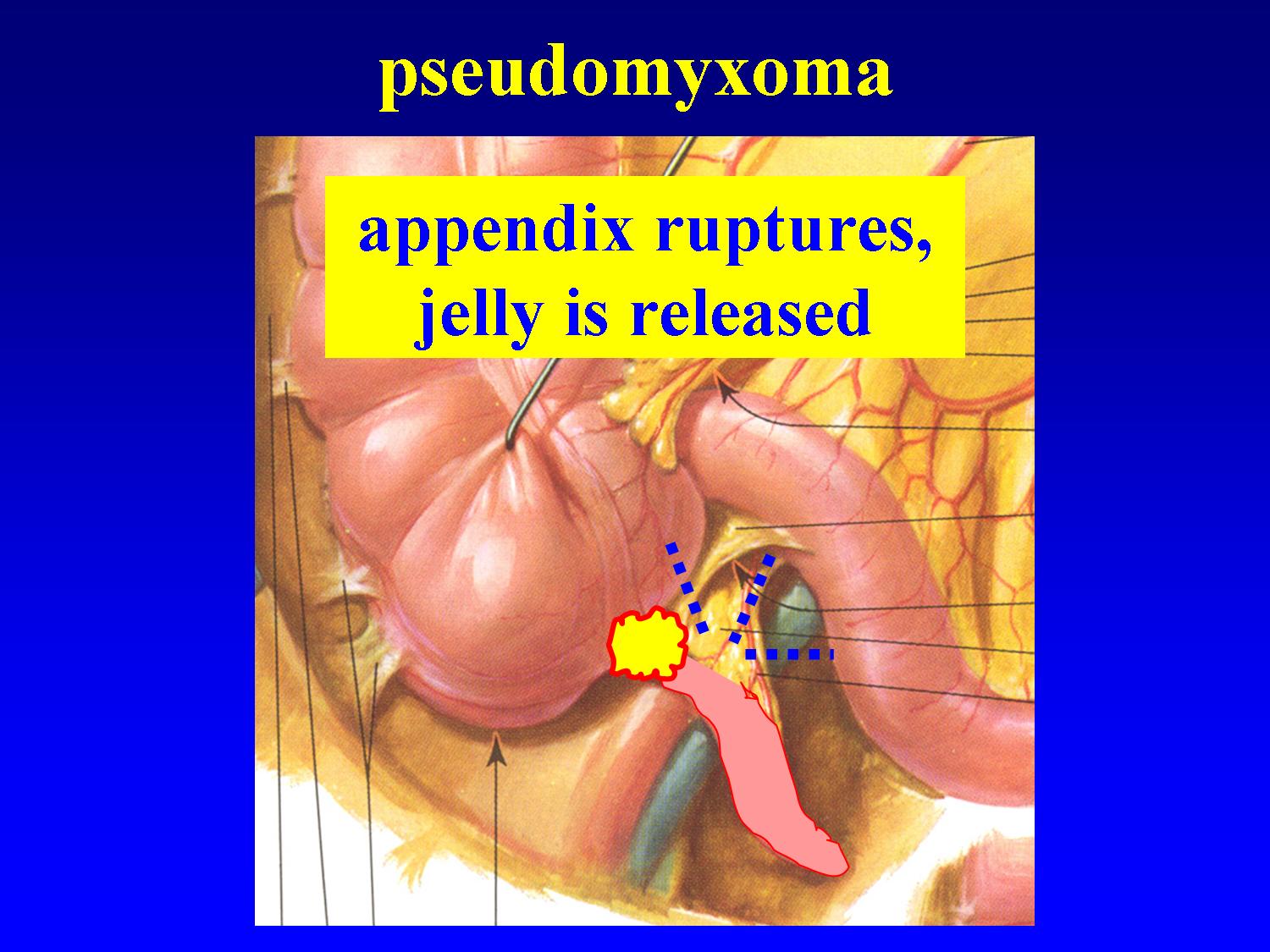
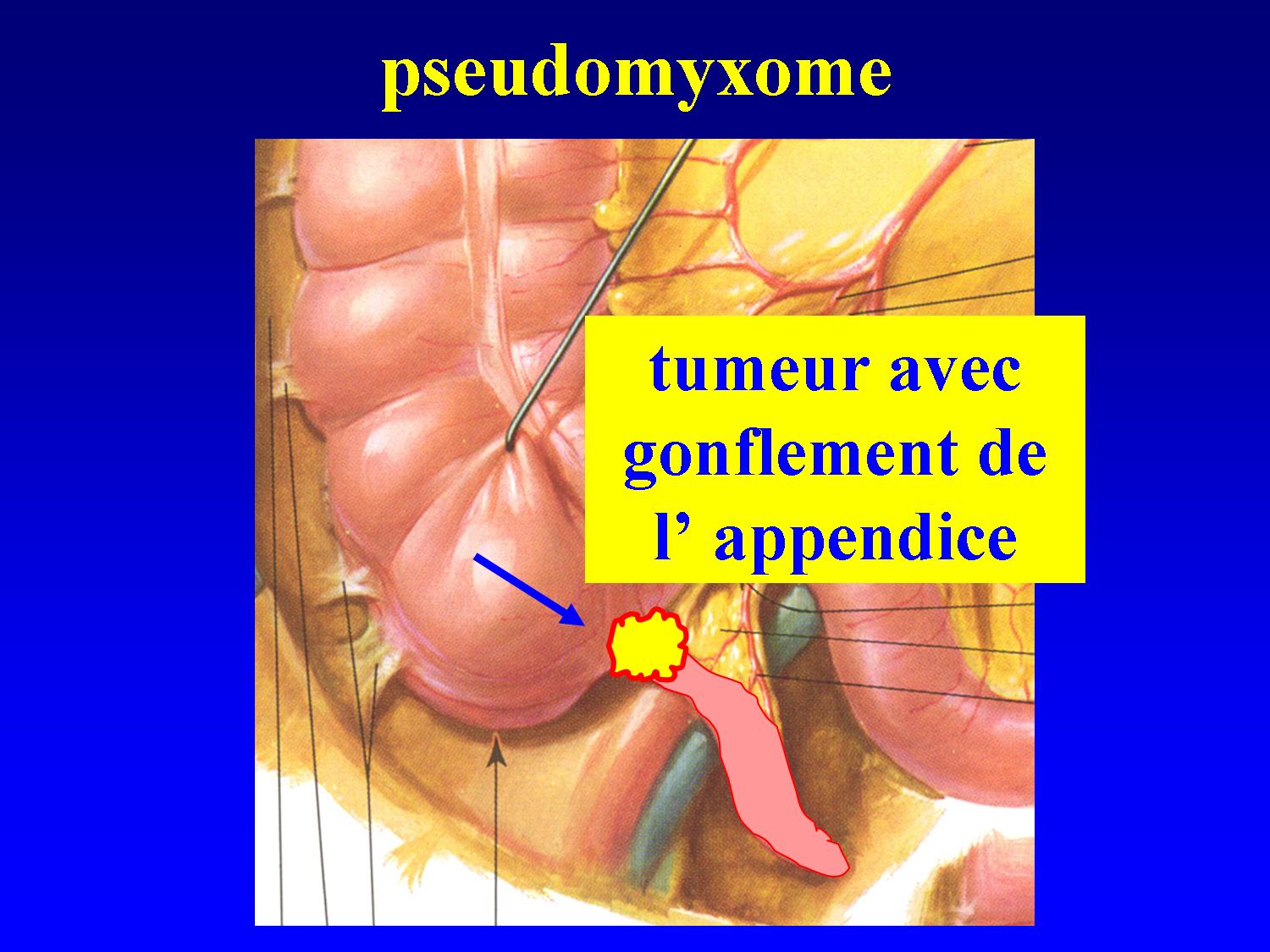
These tumours may disseminate throughout the peritoneal cavity in the form of gelatinous deposits, termed peritoneal pseudomyxoma (PMP). Classification and management of AMT is very problematic for both clinicians and pathologists. Mucocele is a rare pathology of the appendix ranging between 0.2 and 0.7% of all appendectomies. Karl Rokitansky was the first to recognize and describe an appendiceal mucocele (appendiceal mucinous tumour (AMT)) in 1842.

However, our results could still be improved in the future. CRS and HIPEC is a gold standard treatment for PMP with excellent prognosis. Conclusion: AMT is a very rare entity with a considerably good outcome even in disseminated disease. The 5-year overall survival was 100% for the adenomas and 62% for PMP patients. 2 of 8 PMP patients did not undergo CRS ± HIPEC because of comorbidities.
Low-grade appendiceal mucinous adenocarcinoma (AMCa) was diagnosed in 11 patients (44%) among these, low-grade PMP was found in seven cases (28%) and high-grade AMCa was diagnosed in 2 patients (8%). In the histopathologic examination, adenoma was diagnosed in 12 patients (48%) among these, low-grade PMP was found in 1 patient (4%). Another 2 patients underwent CRS and HIPEC 4 days and 3 years, respectively, following initial appendectomy. 15 patients underwent appendectomy only (60%), 5 patients (20%) right hemicolectomy, 4 patients (16%) cytoreductive surgery (CRS) ± hyperthermic intraperitoneal chemotherapy (HIPEC), and 1 patient (4%) appendectomy with caecal resection. Results: Between January 2003 and February 2013, 25 patients had AMT. The calculation of survival rates was performed using the Kaplan-Meier method. Tumour recurrence and the development of PMP was diagnosed based on the patients' complaints, physical examination, imaging studies, and biopsy results. Methods: A consecutive cohort of patients diagnosed with AMT were included in the study. We aimed to evaluate preoperative and postoperative characteristics as well as long-term outcomes of patients with appendiceal mucinous adenomas and peritoneal pseudomyxoma (PMP). Background: Appendiceal mucinous tumour (AMT) is a very uncommon disease.
